|
An update from my blog written on Jan 2011 This is a follow up on my blog written some 2 years ago explaining my experience with nerve entrapment by the illio-psoas muscle. At the time I was uncertain what exactly the cause of my symptoms were. I was just very pleased they were going away. After doing some research and talking to other medical professionals, my experience describes the onset, symptoms, and recovery of a illio-psoas muscle strain and nerve entrapment. Many of the replies to the previous blog appear to be suffering from the same condition. Some however appear to not quite line up with this exact condition. Again I am a personal trainer, not a doctor or physical therapist so I could never give a diagnosis based on a blog reply nor could any medical professional. Other possible conditions and injuries Many of these symptoms line up with other conditions where nerve aggravation is present, but not from muscles or fascia. Commonly these symptoms can be a result of a spinal disc injury. A herniated disc can cause a lot of these issues (http://www.mayoclinic.com/health/herniated-disk/DS00893) as well as other conditions (http://en.wikipedia.org/wiki/Cauda_equina_syndrome [rare]), reproductive issues, cysts or growths. A few replies sound a lot like ostetis pubis (http://emedicine.medscape.com/article/87420-treatment#aw2aab6b6b2) which is a groin injury and more specifically the inflammation of the pubis symphosis. I know personally because I am currently recovering from this caused by a combination of sprinting and being overly tight in the adductors and rectus abdominus. Another future blog will describe this. There is also the possibility of reproductive issues. As you can see, there are a lot of possible injuries/issues associated with these symptoms. Any doctor can start to rule out any of the obvious conditions by getting various tests done. An MRI for the spine would be important to rule out any disc injury or condition. Comments and Replies Some of the replies to my blog are from people who had many tests come back negative and with their doctors having no idea what was wrong with them. Some doctors may blame it on psychological factors or some may just say, “you probably pulled something. Give it some time to rest and it probably will just go away.”. Most of the people reading my last blog had done this already with no success. For those who have gone through multiple doctors and tests, you may want to start to look at a muscle strain of illiopsoas as the primary cause. Others may have this in addition to other injuries which commonly coincide with low back injury. Illiopsoas muscle strain and nerve entrapment The illiopsoas is a muscle that can often contribute to low back and pelvic pain. A strain in this muscle will cause it to tighten up, produce muscle spasms, and create knots/trigger points in the muscle itself or fascia. There is also the possibility of hematoma in the muscle causing issues due the inflammation and enlargement of the muscle. Here are excerpts from Travell and Simmons, The Trigger Point Manual taken from, www.triggerpoint.ca/index.php?p=1_64_Travell-Simons-Trigger-Point ,which has a very good list of relevant excerpts: "ENTRAPMENT may occur because of pressure by the palpable bands of taut muscle fibers that are associated with myofascial TrPs, when the nerve passes through the muscle between taut bands, or when it is compressed between such a band and bone. The cause of the neurological symptoms and signs of neurapraxia that result is easily misinterpreted if this mechanism of entrapment is not recognized." Travell and Simons; Myofascial Pain and Dysfunction, The Trigger Point Manual; 1999; pg. 94. On untrained physician’s diagnosis on an unrecognized condition. "It is all too easy for the physician to blame the patient's psyche for the inability of the physician to recognize the muscular skeletal sources of the patients pain. This wrong assumption can be and often is devastating to the patient." Travell and Simons; Myofascial Pain and Dysfunction, The Trigger Point Manual; 1999; pg. 220 Common for athletes and vigorous exercisers “Good Sport” Syndrome "The “good sport” syndrome is the opposite of hypochondriasis. The “good sport” has a stoical attitude and is determined to ignore pain. He or she charges forth engaging in activities with total disregard, if not outright defiance, of the pain, thereby overloading the muscles and aggravating trigger points. “Good sports” often believe that their pain is a sign of "weakness" and that they must push on to demonstrate their mastery of it. They must learn how this abuse of their muscles contributes to their pain, and how new ways of doing things can let them perform the activities important to them safely and comfortably." Travell and Simons; Myofascial Pain and Dysfunction, The Trigger Point Manual; 1999; pg. 221 Depression and Pain "A major, well recognized contributor to depression is chronic pain. On the other hand, pain may lower the pain threshold, intensify pain, and impair the response to specific myofascial therapy. Patients who have suffered myofascial pain for months or years are likely also to have developed secondary depression and sleep disturbances, and to have restricted their activity and exercise." Travell and Simons; Myofascial Pain and Dysfunction, The Trigger Point Manual; 1999; pg. 110 Trigger Points and Nerve Entrapment by the Iliopsoas Travell defined a trigger point as “a hyperirritable spot in skeletal muscle that is associated with a hypersensitive palpable nodule in a taut band. The spot is tender when pressed and can give rise to characteristic referred pain, motor dysfunction, and autonomic phenomena.” “Acute myofascial pain due to TrPs caused by a clearly identifiable strain on one muscle is, as a rule, able to be fully relieved and normal function restored.” The strain of the illiopsoas muscle leads to the formation of trigger points. These trigger points can refer pain in the classic pattern as shown below. My previous blog talks about nerve entrapment from trigger points. In this situation, the pain will follow along through the nerve pathway giving way to these mysterious pains of many areas. There are a number of nerves passing through and along the psoas that can be irritated. Again www.triggerpoint.ca/index.php?p=1_64_Travell-Simons-Trigger-Point has a great list of excerpts and information regarding trigger points. 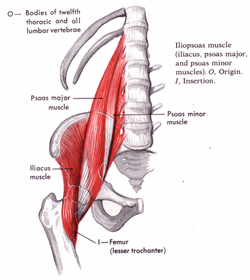 Iliopsoas Anatomy The iliopsoas is comprised of three muscles. The illiacus, psoas major, and psoas minor. They are often grouped together as the iliopsoas muscles because they work together to perform the same functions. They work to perform hip flexion and external rotation, lumbar spine extension, same side rotation, and lateral flexion. The illiacus originates from the iliac fossa and inserts to the lesser trochanter of the femur. The psoas major originates from vertebraes T-12 to L-5 and joins the illiacus to insert into the lesser trochanter. Being that this muscle originates from the lumbar spine, there are many nerves that run in, around, and along the psoas muscle. Nerve roots exit the vertebrae and many branches of these nerves come in direct contact with the psoas. The lumbar plexus, which is a plexus of nerves that includes nerves L-1 through L4 are in fact formed through the psoas. Like all nerves they branch into smaller nerves as you trace it further from its origin. 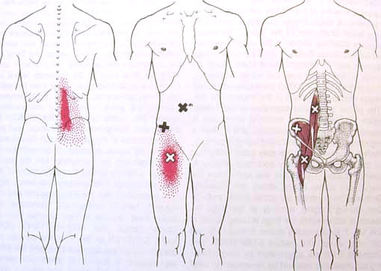 From Travell and Simmons From Travell and Simmons Common Trigger Point Pain Pattern Trigger points can refer pain or other symptoms to other areas as seen in image 2. This is the common referral pattern of the iliopsoas from trigger points. Symptoms can arise in other areas as many people experience. As stated earlier, strain or trauma to the psoas can lead to “knots” or trigger points that irritate the nerves or create pain along the nerves pathway. Describing each possible nerve that could be affected and tracing its path is tedious and lengthy for most readers. Instead of writing on this, below are some possible and common nerves that can become entrapped by trigger points in the psoas muscle and cause pain described in my previous blog. Possible nerves that can be entrapped by the psoas and pain symptoms: Notice the areas that these nerves supply as those are commonly symptomatic areas. From Primal 3D Human Anatomy Regional Edition 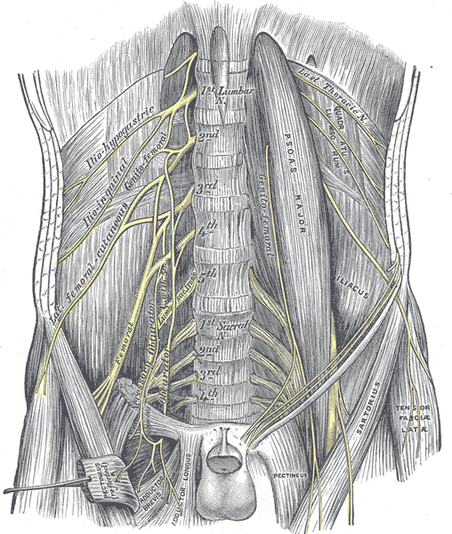 Iiliohypogastric Nerve: Originates from the ventral ramus of the L1 nerve with a small branch from the ventral ramus of the T12 nerve. They "pass inferolaterally through psoas major to emerge from their superolateral border with or above the ilio-inguinal nerves and passes over the anterior surface of quadratus lumborum to pierce transversus abdominis above the iliac crest." It branches into the Lateral cutaneous and anterior cutaneous branches. It supplies the transversus abdominis and internal oblique muscles as well as the posterolateral gluteal and suprapubic skin (the region on the upper/side glute and just above the pubic bone). Ilio-inguinal Nerve: Originates from the ventral ramus of L1 nerve and "emerge from the superolateral border of psoas major with or below the iliohypogastric nerves. Each ilio-inguinal nerve passes obliquely across quadratus lumborum and the superior part of iliacus to pierce the transversus abdominis and internal oblique muscles. Subsequently, ilio-inguinal nerves pass deep to the aponeurosis of external oblique to enter the inguinal canal." It Branches into the anterior scrotal branches for males and labial branches and for females. It supplies the internal oblique muscle the skin of the superomedial thigh the root of the penis and the upper part of the scrotum in males, and the skin of the mons pubis and labium major for females. Genitofemoral Nerve: It originates from the ventral rami of the L1 and L2 nerves "and is formed in the substance of the psoas major muscle where it then emerges from its anterior surface, where it penetrates the psoas fascia. It divides into genital and femoral branches above the inguinal ligament." Femoral Branch It "enters the thigh behind the inguinal ligament" and "enters the femoral sheath lateral to the femoral artery, which it supplies. It then pierces the anterior femoral sheath and the fascia lata to terminate in the skin over the superior part of the femoral triangle." It supplies the "femoral artery and the skin over the superior part of the femoral triangle." Genital Branch It descends "anterior to the external iliac arteries, which gives branches to, and enter the inguinal canals via the deep inguinal rings." In the male, "the genital branches emerge with the spermatic cord, to give off branches to the cremaster muscle, testicular autonomic plexus, and the skin of the scrotum adjacent to the thigh". In the female, they "accompany the round ligament of the uterus to terminate in the skin of the mons pubis and labium major." It supplies the "external iliac arteries cremaster muscle, testicular autonomic plexus, and skin of the scrotum in males. It supplies the skin of the mons pubis and labium major in females." In regard to all the nerves (iliohypogastric, ilio-inguinal, genitofemoral) above this was listed under pathology. The anatomy software had this exact excerpt under each of the three nerves, but I do realize it only menitons the genitofemoral nerve. It is possible this was a mistake in the software because I know there are a number of nerves that can be irritated by the psoas, not just the gentiofemoral nerve. "Parathesis • Because the genitofemoral nerve runs through and on the ventral surface of the psoas muscle, paresthesias of this nerve can result from psoas abscesses or hematomas involving the body of this muscle. • Physically active patients on long term anticoagulation are susceptible to this kind of complication." Other possible affected nerves: Femoral nerve, obturator nerve. These nerves also pass through the psoas, so there is a possibility they can be affected by a psoas muscle strain and knots. I did not experience any symptoms from the areas that these nerves supply so therefore I did not include the details in this blog. There is a possibility that I am missing other nerves or branches of nerves as this can be a complex system. Nerves can be irritated anywhere along its path by a number of tissues. Again, this blog describes the psoas as the culprit. There are many other cases where another tissue can irritate one of these nerves. I have come to the conclusion that my injury was a result of psoas muscle strain which lead to inflammation, hematoma, and/or trigger points. This injury is common to vigorously active exercisers including weight lifters, bodybuilders, American Football and rugby players. It seems as though many doctors would go with a disc injury diagnosis based on these symptoms which is understandable because they can match up. Some of the replies to the last blog strongly point to a disc injury. If the patient was the average sedentary person then most likely it would be a disc injury. Athletes and intense exercisers commonly have disc issues, but if the MRI comes back negative and the patient is goes through physical therapy with a diagnosis of a disc injury, they may be disappointed with failed results. Again, a number of issues have these symptoms but, a psoas muscle strain with these symptoms is quite common among vigorously active exercisers. I suggest finding a doctor or therapist who is familiar with this condition if you suspect you have it. I would stay away from those who look perplexed when bringing up this issue or those who try to steer you in a different direction for recovery. Again, ruling out spine injury and other conditions with these symptoms is a very good idea. In my next blog I will put together a more comprehensive program that I did to recover and what I would do now after discovering the nature of this injury. My first blog exlaining my experience with this issue: Pain, Pressure, Discomfort, Burning, Tingling, and Numbness in the Abdomen, Groin, Pelvic, Genital, and Upper Thigh Areas. My experience with these symptoms as the result of pinched nerves and other underlying issues. For more information on this condition visit www.drgillick.com under clinical issues. He had the only detailed report that was searchable online which may or may not be currently available. References: 1)Travell and Simons. Myofascial Pain and Dysfunction, The Trigger Point Manual. 1999. 2)John H. Gillick MD, MPH, FACA, FACP.. Iliopsoas Muscle Strain - The Filet Minion of Backaches. 2003. www.drgillick.com 3)Van Dyke, Holley, Anderson. Review of iliopsoas anatomy and pathology. Radiographics Jan 1987, vol 7, num. 1. 4)3D Human Anatomy: Regional Edition. Interactive Pelvis & Perineum. 2011. 744 San Antonio Rd. Suite 2, Palo Alto, CA 94303: Breakthrough Personal Training. Expert and professional personal trainer specializing in fat loss, injury prevention, and strength. Psoas function, psoas nerve entrapment, psoas trigger points, psoas pain.
paris brenn
11/13/2013 05:53:39 am
After ALL the websites I've visited, yours had the info I've been looking for- I'm sure I have had an experience w/-nerve entrapment. My L4 &L5 are being treated w/ physical therapy, (det disc & herniated disc) but this morning I woke w/ an electrical type shock pain in my right groin. ouch. It only lasted a few seconds, and I wondered, -what now? At least it has a name and a perfect description here, thanks to you. I will be seeing my doctor soon..Thanks a lot.
Andrea
2/27/2014 01:35:18 pm
Wow! Oh my gosh! I practically want to speak with you if that's even possible! I am a 30 year old female runner and serious weight lifter. I have been diagnosed with meralgia paresthetica (thigh numbness tingling and burning). I felt it slowly come on doing leg press. Anyway, I have been researching like crazy for months and calling doctors and have no where to turn! I have been treated for a slight herniated disc (although there was no X-ray or MRI). Realignments, stim and acupuncture. Only thing that really helps is rest. Then once I do anything, I reaggravate it. Frustrating! I stumbled upon this but can't find your original blog about this from two years ago. Can you direct me to it? Also, if this is a psoas issue causing the nerve entrapment, what do you recommend me doing to treat this?! Please help! First thing I have found that sounds remotely similar to my issue!!! Thank you so much!!!
Jerry
2/28/2014 02:29:08 am
Hi Andrea,
Y1985
4/10/2014 03:29:32 am
Hi jerry,
Jerry
4/17/2014 09:09:07 am
Hello and thank you for your comment Y1985, 4/20/2014 08:56:20 pm
We have been doing an exhaustive data search on paresthesia and are glad to find this. We have started researching a treatment called the water cures protocol. It involves using unprocessed sea salt dissolved in the mouth and drinking an amount of water based on body weight.
Tom
4/22/2014 06:11:33 am
Wow, ok, I believe this is me too. I am 49 years old and have been competing in triathlons for the last 6 years. 10 days ago I did a short triathlon as a start to my season. The run was only a 5K however it was extremely hilly with many steep descents. I did well, went hard, and was completely fine for the rest of the day and night. However, I awoke at 4am to some severe hip pain and I could barely walk or stand the next day! After researching, it did appear that there was some damage to the illiopsoas muscle because it was very tender but also pain and numbness referring down the inside of the thigh, and moving all over the place. It is amazing how different the pain and sensations have felt over the last 10 days. So I guess I am looking for what to expect. I have had acupuncture which seems to have helped but also seems to be a temporary for pain and not for healing. Icing frequently also seems to help relieve pain. My drug of choice has been Aleve which did help but now I am off of that. I am still feeling the tingling, numbness, pain and other sensations down the leg so that is why I kept searching. This blog explains alot. Jerry is there anything more you suggest I do? I do have a great ART Dr near me, Dr Glass in Lake Forest. Maybe I show him this blog? Thanks in advance.
tati
5/12/2014 02:29:23 pm
hi, im an aerial yoga teacher, and the past months i´ve had three students that have experienced numbness on the thighs after a certain pose we practice. this pose is like down dog but we hang from a hammock, the hammock is placed right at the hips, and it very intensely stretches the psoas.
Jerry
5/16/2014 03:52:54 am
Hi Tati,
marco
11/9/2014 11:57:03 am
Hi there I been reading every story I been some seem similar to wat I'm going thru I don't get pain in my growing I get pain on my right side kinda back side of my hip tingling sensation also everytime I go to the gym I suffer from crazy insane pain thought it was my kidney went got blood work and urine sample everything seems fine went to a natural doctor he said I had 2 pinched nerves by my lower back some pain went away but still suffering pain and tingling feeling on my right side doctor just gives me pain meds but I'm depressed have anxiety shortness of breath cause of the pain I need your help what do u suggest I do sometimes I feel like I'm dying if any of u have any info on this injury can you please share or inform me thank u I will appreciate any advice gos bless
Moiz
12/7/2014 05:49:51 pm
Hi,
Leo
1/5/2015 09:01:05 pm
Hi there I wounder if u could help I'm going nuts,two weeks ago I help a friend move lots of boxes I'm only 165 cm 55 kg ok just last week I had to go to the hospital my lower abdominal pain and really sore testicals more on the right tho.ok so they did a urine test and a blood test all clear they did a ultra sound all clear and a ct scan as well all clear and for sti all clear i have been back a couple of times because of the pain it's like Iv been hit in the nut 24/7 and the pain travels to my lower abdominal it's uncomfortable so all Iv been doing is resting like they the said to do take ibuprofen witch I'm doing walking around doesn't help either I'm so confused all test I had done all come back negative witch is good but they did not give me a answer but they it could be a groin strain I have no bruising on my right leg but my groin dose hurt along with my testicals there so sensitive especially underneath please can someone give a answer I'm so not happy with this it's taking over me.
Jerry Yuhara
1/6/2015 12:01:53 pm
Hi Leo,
Jason
1/10/2016 09:34:26 am
Damn, it sounds way too familiar. Mine started with the sensation of a groin pull. No specific activity I can think of to cause it. While driving I was getting a stabbing pain in my hip flexor and in the pubis area. Over the next two days (almost three weeks now) the pain would move from my upper abdomen to my left testicle. It was either in one spot or the other.
Roseann
3/3/2015 10:23:41 pm
I too have had the burning and tingling in my thigh and weakness in lower back. I have a great pT and stopping going due to me feeling good also insurance reasons a. I was doing stretches got up to 7 1/2 miles and bang back to where I started from but with much more lower back pain. I have an appointment with PT today's, will let you know what happens
Jane Kerlin
3/18/2015 09:47:13 pm
This is an in depth analysis of psoas injury. I am five years on with mine. For 7months I have been getting help from a talented osteopath. I need advice on exercises for recovery. I had two caesarians also before my injury. I am on the mend but have some way to go.
Dottie
3/23/2015 03:39:29 am
My PT diagnosis was iliopsoas strain, and says that my back problems DJD and Spinal Stenosis is not causing my pain. My question is will the numbness go away??
Jerry
5/6/2015 08:42:17 am
Hi Dottie,
Abby
4/12/2015 02:12:13 pm
Hi Jerry,
Jerry
4/19/2015 03:34:56 am
Hi,
Albert
4/12/2015 06:25:29 pm
Thanks Jerry for coming up with a good write-up explaining your symptoms and experiences. A small ray of hope after seeing this blog, when I almost gave up with similar pains. In addition to the pain you mentioned, I have pain in the left hand, and coccyx as well.
nigel hatton
4/29/2015 05:29:47 pm
Dear jerry,
nigel hatton
4/29/2015 06:52:37 pm
Jerry,
Jerry
5/6/2015 08:53:04 am
Hi Nigel,
Jerry Yuhara
5/6/2015 08:58:54 am
Hi All,
Simon Byrne
6/2/2015 12:51:52 am
Hi Jerry
Jerry Yuhara
6/3/2015 05:08:51 am
Hi Simon,
Abby
8/14/2015 03:09:09 pm
Were you thoroughly checked for muscle tears/sports hernia? CTs missed my abdominal tears 5 times, MRIs 3. Just wondering. I had a labral hip tear repaired, but the psoas was the main issue and still is. There is a center in Philadelphia that handles surgery for these issues and can more accurately image them.
Paul
6/26/2015 10:34:22 am
Ok so I experienced this on my left leg about two months ago. It's finally better, but definitely still somewhat numb and tingling to the touch. Then while doing yoga of all things (I'm a CrossFitter so yoga is considered active recovery), I lifted my right leg to feel a twinge in my right groin. Felt fine all day but then got home from work and after standing up from my kitchen table, felt extreme numbness.
Jerry
Jerry Yuhara
12/30/2015 10:16:43 am
Flossing is a great way to get the nerve to move within its sheath. Sometimes this type of entrapment can cause similar symptoms as we have all described.
Abby
8/14/2015 03:03:06 pm
Hello, very glad I found this. I was injured in a ground fighting exercise in martial arts after returning with an undiagnosed hip injury, which caused the psoas to spasm. Not realizing this, I put myself into massive back extension and developed a condition that keeps mystifying my doctors. My deep muscles (TA, obliques, often pelvic) gave out, like nothing could hold my body normally, and my back was arched for 6 solid months. My rectus ab eventually tore off from this forced position, which nothing could seem to alleviate. Surgery to correct the injuries was successful, but once I began to work the back again (and fell on the hip, bringing the psoas back into play, likely re-injured the hip) it has all come raging back. HELP!
bri
12/28/2015 11:13:44 pm
I know a fabulous sports ND who works with many Olympians and sports stars in Vancouver, BC. He is extremely talented and not overly priced...his name is Dr Jonathan Berghamer. If traveling is not an option, find somebody in your area who does prolozone or PRP reconstruction. All the best.
Chris
8/19/2015 01:30:13 am
Hello, I injured myself over 3 years ago doing insanity asylum. I have had every test know to mankind and nobody can find anything wrong with me. Immediately after the injury I had pain just left of the navel and it radiated down the left side through the groin into the upper thigh. The pain is and always has been an annoying dull ache. I still have the same pain today just with doing day to day stuff... I have given up all exercise now because the pain is just to bad. I am wondering now if this whole injury could be from the left psoas? maybe a nerve issue? I live in the los Angeles area... just trying to figure this thing out! I have hit my limit with it. Thanks
Paul Fletcher
9/5/2015 05:33:17 pm
Hi Jerry , I had illio femoral bypass surgery , 10 days ago I have all the symptoms described , pain is unbearable , can you suggest any suitable , thing's that I can do to relieve the pain , I have been prescribed Gabapentin , pain is from my abdomen down to my knee , especially sore , inner thigh Many Thanks Kind Regards Paul
Dave
9/11/2015 12:48:14 pm
hi Jerry
Jake
9/26/2015 09:19:56 pm
For years I've gotten this burning pain in my stomach when I run. It gradually went away when I was at my peak, running half to full marathon distance. But I recently had to stop running for 2 months due to an unrelated running injury, and since I started running again, the pain is back with a vengeance. It starts about 10 minutes into a run and gets progressively worse, and the intensity of the pain is proportional to my running effort. The instant I stop and walk the pain stops.
Lou Gallagher
10/19/2015 05:20:10 pm
Hi Jerry.
Henry
11/16/2015 06:39:54 am
Hi Jerry,
bri
12/28/2015 11:09:05 pm
I had tears in illio-limbar, and several SI ligaments on right side from a horse fall. It took a year and a half to diagnose and finally repair with prolotherapy. During that time I had constant neuropathy. Now with it fixed, I still have muscle imbalances and easily rotated vertebrae and joints. Also I have Snapping psoas on both sides, especially left side and very tight glutes. I now have decreased feeling and occasionally numbness in groin/genitals on right side...any ideas and routes to take?
Jerry Yuhara
12/30/2015 10:22:27 am
Hi Bri,
D
12/29/2015 04:16:20 pm
Hi Jerry, I have sensory nerve issues (tingling, deep pain, skin sensations) from the front part of my hip straight down to the top of the knee. I know that front part of the hip flexor is a trigger point. I have had the pain for 6 years now. I did acquire lyme in 2013 which makes the pain very intense. In 2009 I was initially diagnosed w restless legs, then they found b12 deficiency. High dose methylcobalamin b12 shots helped a lot back then. However with the lyme it's now worse than ever. It's the worst while sitting, hence the initial restless leg diag. In 2013 the did find herniation at l4. However a recent MRI done a few months ago revealed no serious lumbar spine issues. It all started after a vigorous hike with very heavy boots that I was not used to with steep inclines. It's bilateral, and I had one dr say it could a
Jerry Yuhara
12/30/2015 10:30:50 am
D,
Jerry Yuhara
12/30/2015 10:48:08 am
Hi Everyone,
Margaret
1/13/2016 10:45:58 am
Hi Jerry,
Harry
2/11/2016 04:45:37 pm
Thank u, thank u n thank u. I feel like crying from this information I have found. It's hit the nail on the head. STILL NOT SURE WHAT EXACTLY I HAVE THOUGH N WHO TO GET HELP FROM. I have had many issues with my groin, testicles, lower abs n more. I've had two key hole surgeries, which was for a mesh n both my testicles. I have been suffering now for over 14 years. It all start with hard use of amphetamines n I noticed a big change down below n that's when all problems started. A Physio told me I was full of pressure points n adviced me to do yoga coz need lots of stretching. She said I was full of pressure points, full.... There is nerve damage also I'm sure. I've tried swimming, biking, pull up bar, karate n much more but still have problems n it's always there. Now I've stopped doing everything so I can see what is going on. Reflexology also helped me but have not done it for years. The only thing I cN think of that will help is yoga m reflexology. If u need more info to better advise me then please let me know. Thanks
Jerry Yuhara
2/22/2016 03:26:26 pm
Harry,
Tammy Morgano
3/30/2016 09:08:45 am
Two years ago in February I had a pelvic ultrasound done due to a burning crampy feeling in my lower abdomen and irregular periods. I had cyst on my ovary and was told to watch and wait. Two days later I was in excruciating pain and went back in a week and had another ultrasound and the cyst had grown but was told that should not be causing the pain. I went to another obgyn and was told due to the size and pain I was in I should have it laparoscopically removed. The sugery was in April 2014. They removed the cyst and my Fallopian tubes and the pain was still there. Since then I have had a colonoscopy. X-rays and MRI's, countless bloodwork, pudental and superior hypo gastric nerve blocks, Ovarian vein embolization, done three rounds of PT and seen three chiropractors and the pain is still there. I've been on gabepentin and lyrica which helps. I've also had some luck with dry needling but my physical therapy visits ran out already. From all the posts I've read and reading your information I believe this is what the problem could be. The original pain started with a knot like feeling pulling above the pubic bone and below the belly button front and back and radiating down through my thighs. It never felt muscular until it spread all through my whole trunk back and front. I use a hot tub and hydromassage 5 to 6 days a week to try and get some relief. Not one doctor has suggested this problem.,.
Christian
3/31/2016 01:48:46 pm
Dear Jerry
Jerry Yuhara
4/7/2016 09:29:34 am
Hi Christian,
Owen
7/13/2016 11:41:34 pm
I have your symptoms in addition to facial numbness and spasms throughout body. Are there enough nerves down there to account for that too?
Jerry Yuhara
7/14/2016 03:31:13 pm
Hi Owen, Comments are closed.
|
AuthorJerry Yuhara, CPT, CSCS, CMT #75123 Categories
All
JY Fitness
299 California Ave, Suite 120 Palo Alto, CA 94306 650-485-1240 contact@jyfit.com Contact Copyright JY Fitness 2024, All Rights Reserved. Find us on Nextdoor.com
|